
Theme 5: Integrating the care
Reform North
The Reform North programme previously known as Renewing Our Vision was given a fresh brand in 2023 reflecting the importance of staff and service users being at the heart of Reform.
The Reform North Programme comprises ambitious plans for reform and transformation for the Trust The programme is divided over 7 workstreams with associated distinct and interdependent projects. All are focused on how we improve the services we deliver, ensuring that we are adapting to the changing needs of our population.
In 2023, the Trust saw the successful reconfiguration of maternity services on the Antrim site.
Work was also commenced to review emergency and general surgery services, engaging widely with stakeholders to prepare options for public consultation on the future of the service.
A vision for Causeway hospital was delivered. This was developed though engagement with staff, which was formally launched in March 24.
Work on an intermediate care model has continued throughout 2023/24, with a range of options to be considered to optimise provision of services for assessment and rehabilitation and enhanced care across all of the Trust’s community hospitals and care facilities, as well as developing our plans to strengthen home care (formerly known as domiciliary care).
Through the Elective Reform group steps are being taking to address the growing demand and long backlogs in Trust waiting lists by exploring alternative pathways for service users and looking at innovative ways of modernising outpatients and inpatient/daycase provision.
The Cancer Strategic Board has been re-established, focusing on specialist areas and tumour sites to understand the challenges and opportunities for reform to improve outcomes.
Further work continues in the areas of Unscheduled Care, Mental Health and Learning Disability and Children’s Services aligned with regional strategies and local action plans.
Vision for Causeway
In March 24, the Trust publically launched its Vision for Causeway hospital. The vision document was developed following a series of staff engagement workshops where the Trust outlined their ambitions and aspirations for the future of the hospital. Causeway hospital has so much to be proud of, with over 500 people benefiting from its services on a daily basis and the Trust wanted to ensure that this was reflected in the document.
The vision reiterates the Trust’s commitment to a 24/7 Emergency Department and acute inpatient services. It is acknowledged that Causeway is, and will remain, an acute hospital with services for both adult and children. The vision explains the Trust’s intention to build and strengthen the services that are provided there. The Trust recognises that Causeway will continue to thrive by working in partnership – with primary and community care, with the community, voluntary and independent sectors, with the NI Ambulance Service and others.
The Trust’s ambition for the hospital covers a number of areas where the Trust believes it can build services and attract investment.
- Same Day Emergency Care – In Causeway, the Trust has recently received an investment of £1.8m to develop urgent and ambulatory pathways. Ambulatory or same day emergency care means getting patients who need senior medical assessment, diagnostics and/or treatment to that care without going through an Emergency Department or spending a night in hospital
- Integrated care – The Causeway locality can lead the way in providing integrated care as part of the regional development of the Integrated Care System. As services are developed in the hospital the Trust will work with its partners in primary and community care, and the community, voluntary and independent sectors, to provide joined-up care to the Trust’s population
- Elective Care – Alongside its focus on unscheduled acute care, Causeway is well positioned to deliver elective services. The Trust’s ambition is to see Causeway operate as an elective and diagnostic hub for the northwest, delivering services to patients from well outside its natural catchment area
- Mental Health – The development of Birch Hill, the new inpatient mental health unit in Antrim, gives the Trust an opportunity to rethink and reshape how it provides mental health services in Causeway, in line with the Regional Mental Health Strategy
The Trust firmly believes that Causeway has a bright future as part of its acute hospital network and as a key player in health and social care provision for the local area. By focusing on the right things, attracting investment and building the workforce, the Trust is confident that Causeway can continue to serve its population for many years to come.
Integrated care system
The Integrated Care System (ICS) is a new framework for how health and care services in Northern Ireland is planned. It is a single, joined-up system, based on the different parts of health and social care, and others who have a role in the wellbeing of the population of Northern Ireland, coming together to understand what it is that is needed, and how this can best be delivered with the resources available. At the heart of the ICS are five Area Integrated Partnership Boards (AIPBs), each covering an HSC Trust area. The Southern AIPB ran as a test throughout 2023/24, with plans in place to establish the other four areas during 2024/25.
Trust / GP Partnership
The Trust / GP Provider Partnership continued to meet regularly throughout 2023/24 and has progressed with its agreed work plan. This has included the rollout of Direct Access Physiotherapy across the Trust area, and developing a role for Trust clinicians in GP Federations’ educational meetings. The Trust’s elective care reform programme has benefited greatly from GP involvement, including the development of waiting list guidance for patients in response to a recommendation from the Northern Ireland Public Services Ombudsman (NIPSO). The Partnership’s focus during 2024/25 will increasingly move to the rollout of the encompass system, and how this can improve communication between primary and secondary care.
No More Silos
During 2023/24, the Trust secured significant investment from the No More Silos (NMS) Programme. Aimed at integrating Urgent and Emergency Care, the funding prioritised three key areas: Rapid Access Pathways, Urgent Care Services, and Phone First. As a result, new services have been established, including the Acute Ambulatory Unit and Surgical Assessment Unit at Causeway Hospital, which provide same-day acute care for medical and surgical patients. Additionally, rapid access Respiratory and Cardiology pathways have been developed at Antrim Hospital. Clinical Communication Gateway (CCG) Hubs have also been implemented at both acute sites, facilitating streaming for CCG referrals. Increased efforts to promote the Phone First service have led to higher call volumes. Moving forward, these services will continue to be embedded and optimised in 2024/25.
Population Health
Population health tackles the underlying causes of poor health and health inequalities. Initiatives such as the Healthy Lifestyle Partnership’s Causeway Healthy Kids Project are delivered through partnership, bringing together a wide range of expertise and resources. The project involves education and activities on nutrition, mental and physical health, and has reached over 1,000 children. Winning the population health and overall categories in the Advanced Health Care Awards has energised roll out across the Northern Area.
Partnership working is key to success in population health and the Trust was recently involved in sharing learning on the Thrive project, which it Co-Chairs. Thrive is a multi-agency and cross sector initiative focused on the wellbeing and educational attainment of children and young people experiencing health inequalities in the Newtownabbey area. Population health initiatives often involve the sharing of resources across Government boundaries. Thrive is funded through an innovative Collaborative Investment model where 7 Government Departments and agencies pool funding, achieving much more than we could separately. Together with the Trust’s Learning Partner, Stranmillis University College, a 2-day conference event explained why the place based approach for Thrive has been a success. The event included a session on the partnership funding model, with input from the Minister of Finance and Auditor General for NI, and a panel discussion on how the Collaborative funding model works to deliver better outcomes for local children.
Population health involves building understanding of our population and consideration of how our services are geared to meet the needs of specific populations. Our Rurality Framework focussed on the needs of rural dwellers and assessed how our services were delivered in ways that met their particular needs. There are many examples of services which focus on rural needs and this is being enhanced as we further develop our understanding of rural needs. The launch of the Trust’s Rural Framework celebrated its successes to date and challenges us all to consider how our services can be adapted to work for the 42% of our population who live rurally.
The Trust’s commitment to work in partnership with others to achieve better outcomes for shared populations is necessary to achieve quality improvements where complex and underlying factors result in health inequalities. Through involvement in a range of initiatives like these examples above, the Trust is building its learning and success providing a strong foundation as it moves forward with establishing a Population Health Committee of Trust Board to oversee and further develop population health approaches as essential elements of service delivery across the Northern Area.
Mental Health
Greatix
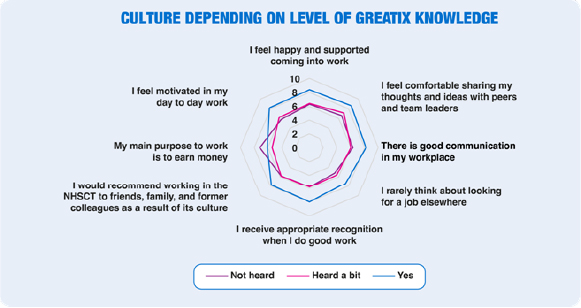
Over the last year the Mental Health, Learning Disability and Community Wellbeing (MHLDCW) Division have placed a focus on GREATix (born from the Learning from Excellence movement) as a way of saying Thank You when staff go above and beyond what is required from their role. The aim is to value, recognise, and perpetuate excellence in recognition of these deeds. Following the successful introduction of this staff feedback tool in the Psychiatric Intensive Care Unit in 2021, its potential to support staff morale has been extended across the entire Division through ongoing promotion and responding to nominations in a way that matters to staff. “I think the fact that the certificates are signed by a director shows staff that what they have achieved is being heard about by Senior Management Team, which is positive”. Analysis of staff feedback indicates that many staff have changed, or intend to change, their practice having seen how they have directly contributed to excellence in patient care, and to the supportive Team North ethos: “I feel that it has encouraged me to consider others for nominations but also to elevate how I work to try to continue to work to that standard’.
Community Wellbeing Service
Providing financial wellbeing support for staff required a significant culture shift given the stigma around the matter and many staff and managers did not necessarily recognise this as a critical part of staff wellbeing which impacts on care delivery. If they did, they were often unsure about what to do about it. A commitment to bring about a culture change was included in our Financial Wellbeing Action Plan and significant progress in what is always a challenging objective has been achieved. Initiatives such as Talk Money week and Northern Saver newsletter, have helped create a culture of openness with lot of practical advice and staff sharing their top saving tips. The Trust’s food bank referral scheme provides immediate practical support for staff in crisis with food and follow up debt management support. This ensures a more confident culture as managers know that they can offer practical support when staff approach them. Culture change involves educating staff on the importance of taking care of their finances and acting on it, including planning ahead. The demand for the free wills service has grown from 100 last year to 800 this year, showing a depth of culture change. A recent survey of staff on their financial issues received a greater response than our original baseline survey, with almost 1,000 responses. The Trust has led regionally on Financial Wellbeing and have recently been recognised as one of the first Financial Wellbeing Champions in the national scheme awarded by the UK Government arm’s length body dedicated to expanding financial wellbeing.
Health & Wellbeing
The Trust recognises that mental health and wellbeing of staff is a key concern for managers and staff colleagues alike. The Health and Wellbeing service received funding from NHS Charities Together to deliver a programme where we strengthened understanding on both prevention, utilising Take 5 as a tool for good mental wellbeing and building resilience, and on early intervention, through learning on mental health first aid and similar training programmes. Teaching self-care is a key component of this programme; by looking after yourself, you are better able to look after others, both colleagues and service users. To ensure this provides a more capable workforce and to achieve maximum reach, we adopted cascade approach to sharing learning. Amongst the almost 2,000 staff upskilled, the Trust now has Take 5 Ambassadors and Mental Health Connectors amongst our workforce, bringing shared knowledge and skills to service teams across the Trust. Staff are supported with both virtual and physical resources to help them bring this strengthened capability to their colleague.
Psychological Services outcomes framework
Psychological Services routinely gather and analyse outcome measures. This allows services to monitor the safety, effectiveness and appropriateness of interventions and also helps identify any gaps in service provision and performance. The data also permits services to gather practice-based evidence for the interventions offered and evaluate the effectiveness of treatments.
Since 2016, the agreed framework used across Psychological Services in NHSCT is McCusker’s (2014) “Three Pillars Model”. This evaluates clinical outcomes across three areas:
- Access
- Acceptability
- Effectiveness
Access evaluates whether the profile of clients within the service matches the intended population of the service. Acceptability is a measure of service-user and clinicians experience of the service. It measures perceptions on how treatment impacts on overall wellbeing and social/psychological functioning. Effectiveness measures the impact of treatments on recovery for individual service users, which is measured through symptom reduction and clinical outcomes including quality of life, work and social functioning, and improvement in well-being.
During 2023/24, outcomes gathered during 2022/23 were analysed and a visual report was developed.
Diabetic Prevention Programme
The Trust Diabetic Prevention Programme is an evidence based and NICE compliant programme, which provides 18 group sessions over 9 months where health coaches inform and motivate high-risk pre-diabetic service users to change their lifestyle and reduce their risk. With over 1,200 people completing this programme, 1 year later, evidence outcomes show 80% of people with reduced haemoglobin blood test levels, over half of which are no longer at risk of diabetes. 74% of people show weight loss within a year of starting the programme.
The evidence of the impact of heath coaching has been used to pilot a Weight Reduction programme with Health and Wellbeing Team with the Trust respiratory Team, particularly the Sleep Apnoea service. Outcomes were positive with 82% retention rate on the 12-week programme and 80% of participants experiencing weight loss.
Given the strong outcomes achieved, the Trust intends to continue working with the Respiratory/ Sleep Apnoea team to run another Weight Management group and also pilot this service with referrals from primary care in the Causeway area through primary care.
As with our experience with Diabetic Prevention Programme, there will be learning from each group and adaptations to make, which strengthens the programme and potentially this innovative health coaching model could be rolled out to other areas including staff working within the Trust.
Learning Disability Day Services
The Trust’s Learning Disability programme has recently gained the licence to work in partnership with the Duke of Edinburgh’s Award scheme. This is an excellent opportunity to open this award to young people with learning disabilities by supporting service users to build confidence and realise their potential, all while gaining recognition for their wonderful and unique skills. This scheme will be piloted in the Ballycastle area in the first instance with the hope that its success will widen this opportunity for all young people with learning disabilities in the Northern Trust area.
Learning Disability Services Day Opportunities have also unveiled the new Ballycastle Base, which moved closer to the seafront. This move is designed to enhance independence for the service users by providing easier access to their local community. To celebrate this exciting development, a special open day for staff, service users and carers was held and it was an honour to welcome Councillor Ciaran McQuillan, the Mayor of Causeway Coast and Glens, as a special guest.
Community Wellbeing
Integrated care involves strengthening how service users can play their role in looking after themselves. The Trust’s service users significantly benefit from many health and care interventions. The Trust also recognises the role that enhanced self-help can offer to many in navigating both services and community supports. Empowering people, carers and their family to manage their conditions alongside the services the Trust provides is an important way of ensuring service users are fully involved in their own care and recovery. It requires accessible and reliable information made widely available and easy to use. Population Plus provides a publically accessible and live directory of local services, searchable by condition and by postcode, containing details on over 850 interventions. People can use Population Plus to identify what supports they can access locally.
Within the first quarter of 2024, this directory has been accessed by 1,103 users, viewing 51,934 pages between them. 19% of users to Population Plus are returning users. 80% of people sampled stated the directory was easy to use and 100% found the information useful. Service pathways have been developed which integrate use of these local supports into care provision by the Trust. Where needed, Connect North Link Workers can help individuals develop and enact their support plan through an integrated and holistic assessment. Within the first 20 months almost 1,600 clients have been referred for one-to-one support and Trust link workers have delivered more than 18,000 interactions with clients including 2,682 signposts and 1,070 social prescriptions. The top reasons for referral include dementia, groups and activities, befriending, loneliness and isolation and mental health.
Social Work and Social Care
During this reporting period the Trust has maintained its responsibilities for exercising, on behalf of the Department of Health (DoH), the statutory functions which are directed by virtue of authorisations made under the Health and Personal Social Services (Northern Ireland) Order 1994 (the 1994 HPSS Order). The Trust has continued to meet its statutory obligation to put and keep in place arrangements for monitoring and improving the quality of social work services, which it provides to individuals and the environment in which it provides them.
Reports are presented twice yearly to Trust Board regarding the Trust’s Annual and Interim Statutory Function compliance this includes the 6 monthly Corporate Parenting Report. There are mechanisms in place within the Trust to assure that professional leadership and the control and management of professional and regulatory issues pertaining to the statutory functions are reviewed at regular intervals. The Trust has a Social Care Governance forum which takes place 8 months of the year, specifically focusing on the delivery of statutory functions, areas of development, improvement and risk relating to statutory functions are progressed at this forum.
In addition to the above and in compliance with the Trust’s arrangements for monitoring Directed Statutory Functions (DSF), the Executive Director of Social Work provides overview reports and presentations to Governance Committees and Trust Board on any new or emerging risks that impact detrimentally on the delivery of statutory functions. Divisional and Corporate risk registers are also utilised to capture specific issues pertaining to the delivery of statutory functions. This process is utilised in order to identify the regional and local challenges, the mitigations and monitoring in place to address these challenges and to notify Trust Board on how these challenges have been appropriately escalated to the Strategic Planning and Performance Group (SPPG).
Assessment of the Trust’s performance in effectively and efficiently delivering directed statutory functions
This reporting period has continued to be a very challenging one where demand has increased at the same time as an unprecedented staffing shortfall. Emerging pressures and risks that continue to affect our statutory functions are outlined below:
There are 2 core themes impacting all areas of Social Work:
-
Inappropriate Placements in Adults and Children’s Services
The continued and growing pressure on the looked after children system and in particular on the availability of placements has resulted in an increase in the number of children in inappropriate placements. On occasions the Trust is unable to meet the demands for specialist bed based placements within our Adult Services programmes, this results in bespoke placements being designed within a community setting, trackers are in place within Children’s and Adults services to monitor these arrangements closely.
-
Workforce Challenges
Social services have experienced significant workforce pressures during this DSF reporting period, which have impacted on the capacity of the Trust to discharge statutory duties. The current workforce arrangements present a significant challenge. This is also in the context of increasing demand for services. Recruitment of social work staff in particular areas of social services is difficult. Where teams are staffed well there is a disproportionate number of newly qualified staff. The Trust has put in place strategies to recruit and retain staff including introducing new recruitment pathways, different skill mixes, additional administrative support, and mentoring / coaching networks for frontline social workers.
Statutory function challenges within Adult Services
Approved Social Work
Despite there being no increase in Approved Social Work (ASW) assessments compared to last year, the service remains under considerable pressure due to lack of inpatient beds, delays in ambulance and PSNI attending, and the emergence of issues relating to the Regional Emergency Social Work Service (RESWS), including difficulties with handovers to and between the daytime service and the RESWS. The Trust ASW service has remained under pressure during the reporting period. Whilst the number of local referrals has not increased significantly, the number of admissions has increased by around 20%. The ASW lead in the Trust is continuing to work alongside SPPG and DoH to explore solutions to these issues.
Unmet need for Domiciliary Care
The report indicates that the Trust continues to have a significant level of unmet need for Domiciliary Care. This level of unmet need spans all programmes of care with older people being the largest group affected making up 80%. Maximising capacity in domiciliary care is a core focus for the Trust Community Care Division and reform work continues to take place within one of the new DoH Social Care Reform Collaborative work streams.
Adult Safeguarding
The quarterly data submitted to SPPG provides detail that adult safeguarding services has seen a significant increase of referrals during this reporting period. The greatest number of referrals received relates to people with mental ill health, with older people being the second largest grouping followed by people with learning disabilities. The Trust does not currently face any challenges with their delivery of statutory functions with respect to adult safeguarding. The Trust has a governance structure and reform board in place to monitor adult safeguarding arrangements and deliver improvements.
Carers Assessment
Carers play an important role in the provision of care and support they provide to a family member or someone close to them. The Trust remains committed to the promotion and uptake of carers assessments, using a standardisation of approach of the Northern Ireland Single Assessment Tool (NISAT) and Carer’s Conversation Wheel, across all Programmes of Care.
Unallocated cases in Older People and Physical/Sensory Disability Services
Due to increased demand, the Trust’s Community Care Division has experienced a new challenge around unallocated cases. Presently these unallocated cases are managed through the duty Social Work (SW) system. The Trust continues to engage in regional discussions surrounding the definition of unallocated cases in Adult Services; in addition to this, the Trust continues to develop an improvement plan and a governance assurance system to effectively monitor unallocated case activity. This issue has been added to the Divisional Risk Register.
Annual care reviews
This area continues to be an issue, particularly across older people and learning disability services. The cause is largely related due to increased workloads, increased referral levels along with the prioritisation of adult safeguarding, hospital discharge and Mental Capacity Act work.
Interface with service delivery process
A number of DSF challenges are also included in the Trust’s Service Delivery Plan (SDP). These services relate to:
- Adult Day Care
- Adult Short Breaks
- Domiciliary Care Hours
- Mental Health Services (Adult Mental Health, Psychological Therapies, Dementia)
- Mental Health Acute Bed Pressures
Statutory function challenges within Children and Young People’s Services
Unallocated cases
Trust reporting procedures for unallocated cases indicate an improved position in our Gateway services, a continued challenging position in our Family Support Teams and an unprecedented position in our Looked After Children’s Services. An improvement plan is in place for all unallocated case activity within the Trust. The Trust continues to report Gateway and Family Support unallocated case activity via the agreed SDP reporting procedures.
Increase in looked after children
Since 2021 statutory functions reports for the Trust highlight a very significant increase in its looked after children (LAC) population. As at the end of March 2024 there were 807 within the Trust, an increase of 43 young people since the submission of our Interim Corporate Parenting data in October 2023. The Trust’s LAC service has now experienced an increase of 118 children since the end of March 2020. Inevitably the increase in looked after children has resulted in increased demand for suitable placements, and challenges in completing statutory reviews/visits.
The increase in kinship placements is positive and in line with legislation, policy and research findings. The Trust continues to support children to remain with family or friends. This trend has changed the face of foster care as kinship carers often need different and/or more intensive support. The arrival of increased numbers of separated and unaccompanied asylum children into the looked after system has added challenges for the corporate parenting system within the Trust.
Children with disability, short breaks
The Trust continues to record pressures in this area, and notes that services have had to be re-purposed to provide residential accommodation for children with a disability who become looked after. There have been improvements in the Trust’s short break performance with the 2022/23 action surrounding Children with a Disability being closed by SPPG in October 23. In this reporting period, the Trust has placed significant focus on the transfer of operational ownership of a residential short breaks facility in one area of the Trust whilst also profiling and expanding other types of short breaks.
Interface with children’s strategic reform board
The Children’s Strategic Reform Board under the leadership of DoH has been set up to tackle many of the key issues for children services by working creatively and collaboratively with Trusts and other stakeholders to assess the issues, underlying causes, and develop robust and creative plans to tackle them. Associated work streams under the Reform Board will be focussing on a number or areas that are also included in the Trust’s DSF action plan; these include unallocated cases and placement pressures.
Summary of areas where the Trust has not adequately discharged their directed statutory functions
Following end year accountability with SPPG, the 2023/24 DSF Action Plan for Northern Trust was closed. Of the 22 actions, 4 were completed and the remaining 18 actions have been carried across to the 2024/25 DSF Action Plan. Commissioning leads within SPPG, having reviewed the DSF reports and following discussion with Trust leads, agreed that one new action would be included in the 2024/25 Action Plan – unallocated cases in Older Peoples Service.
The 19 actions in the 2024/25 DSF Action Plan forms the basis of ongoing quarterly accountability meetings between SPPG and Trust SW Assistant Directors. As noted above these actions are crosscutting with a focus on placement pressures, unallocated cases/unmet need, care management reviews and workforce.
Social work safety and quality improvement priorities (SQIP)
There are formal mechanisms in place within the Trust to provide assurance that professional leadership and the control and management of professional and regulatory issues pertaining to the social work are reviewed at regular intervals. The Trust has a Social Care Governance Forum which takes place 8 months of the year specifically focusing on professional governance. Areas of development, improvement and risk relating to Social Work are progressed here.
Emerging pressures and risks associated with Social Work services are escalated regularly through the Trust’s integrated assurance framework via the Assurance Committee, which is a standing committee of the Board of Directors & Trust Board. The purpose of the Committee is to review the effectiveness and reliability of the Trust’s assurances regarding governance arrangements, risk management and the control environment. The Social Work SQIP was introduced in 2023/24 with an aim to confirm the comprehensiveness of the six priorities identified below to the Outcomes and Assurance Committee.
The Assurance Committee will provide a third line of assurance on the Social Work SQIP within the Trust’s Integrated Governance and Assurance Framework. It can ensure that robust governance, risk management and assurance processes are in place across for the SW SQIP to promote the delivery of key objectives.
Within Social Work services we understand that many high performing organisations are now moving away from standalone Safety/Quality/Governance/Improvement functions to a more integrated whole systems approach to quality. Whole system quality comprises integrated quality planning, quality control, and quality improvement activities that inform an organisation-wide, interlinked, and strategic approach to improving the quality of services provided by an organisation. The Trust is embarking on a design process to determine how different functions within the organisation can be woven together in a more integrated manner with this aim in mind.
The Social Work SQIP has been designed, with a focus on six key priorities for improvement over 2024/25. This will contribute to the strengthening of the social work functions of quality planning, quality control and quality improvement within the Trust, with targeted focus on these six key areas in the first year of this approach.
World Social Work Day celebrations
The Trust was delighted to host a conference to celebrate World Social Work Day in March 2024. Executive Director for Social Work in the Trust, Maura Dargan, opened the event and welcomed Social Workers and colleagues from across the Trust and partner organisations.
Speakers for the day included Professor Deirdre Heenan, Professor of Social Policy, Ulster University and Alex Kane, newspaper columnist and political commentator.
Delegates welcomed the opportunity to hear from a range of inspirational speakers and visit the many exhibitions and information stands from organisations such as the Regulation and Quality Improvement Authority, Northern Ireland Social Care Council, British Association of Social Workers and others. The event was brought to a close by Executive Director Maura Dargan who reflected on the challenges faced by Social Workers over the previous few years and thanked them for their significant contribution.
Annual health checks
Enhanced services by GPs, which includes annual health checks for people with learning disability, were reintroduced in April 2022, but then suspended from December 2022 until March 2023.
Trust Healthcare Facilitators (HCFs) have continued to engage with GP practices and by doing so they have ensured that the GP registers for people with learning disability are kept up-to-date. The HCFs completed some health checks across the Trust, either in service users’ own homes or in a clinic setting. Other settings are considered depending on the service users’ needs and wishes. During the reporting period, 947 health checks were completed by GPs and 125 were completed by HCFs. The HCFs continue to liaise with GP practices and work closely with them to ensure that annual health checks are completed in a timely fashion.








